Strong,
inescapable, and temporary stresses trigger similar responses
to those caused by an illness: fever, sleepiness, decreased
appetite & sex drive
Brief stress
causes SNS arousal and HPA Axis arousal: in the short run,
these strengthen the body.
Long-term or
chronic stress, anger, or anxiety leads to harm of the body,
e.g.,
- Prolonged
cortisol release seems to limit the synthesis of immune
system cell proteins, e.g., people living near the
Three-Mile Island nuclear plant accident (1979) over the
subsequent year had decreased immune system cells
- Antarctic
researchers over 9 months of cold, dark, and isolation
show reduced T-cells functions (ca. 50% of
normal).
- Exposure
to common cold viruses does not lead to increased illness
for those subject to less than a month of stress;
individuals with 4 or more weeks of stress are more
likely to become sick.
- Recent
research of children who had been subjected to severe
child maltreatment by their parents by the age of 3
demonstrated significant negative alterations
in the overall connectivity patterns
in the development of the white matter of their
brains (as compared to matched control children;
Puetz et al., 2017). The researchers note that such
findings are in line with research showing that high
levels of HPA axis activation and chronic exposure to
cortisol affects neural development in
children.
- Chronic
stress may increase the likelihood of developing
cancer (Dai et al., 2020; Tausk, 2023) including the
spread of breast cancer to the bones (Lourenço
et al., 2022)
References
Dai, S.,
Mo, Y., Wang, Y., Xiang, B., Liao, Q., … Zeng, Z. (2020).
Chronic stress promotes cancer development. Frontiers in
Oncology, 10, 1492. https://doi.org/10.3389/fonc.2020.01492
Echouffo-Tcheugui,
J. B. et al (2018) Circulating cortisol and cognitive and
structural brain measures. Neurology, 91(21). https://doi.org/10.1212/WNL.0000000000006549
Lourenço, C., Conceição, F., Jerónimo, C., Lamghari, M.,
& Sousa, D. M. (2022). Stress in metastatic breast
cancer: To the bone and beyond. Cancers, 14, 1881. https://doi.org/10.3390/cancers14081881
Ouanes,
S., & Popp, J. (2019). High cortisol and the risk of
dementia and Alzheimer’s disease - A relview of the
iterature. Frontiers in Aging Neuroscience. https://doi.org/10.3389/fnagi.2019.00043
Puetz, V.
B., Parker, D., et al. (2017). Altered brain network
integrity after childhood maltreatment: A structural
connectomic DTI-study. Human Brain Mapping, 38(2),
855-868. https://doi.org/10.1002/hbm.23423
Tausk, F. (2023). Psychoneuro-oncology: How chronic stress
grows cancer. Clinics in Dermatology. https://doi.org/10.1016/j.clindermatol.2023.03.008
Wirth,
M., Lange, C., & Huijgers, W. (2019). Plasma cortisol is
associated with cerebral hypometabolism across the
Alzheimer's disease spectrum. Neurobiology of Aging, 84,
80-89. https://doi.org/10.1016/j.neurobiolaging.2019.08.00
![[Brain Image]](../graphics/head_space.gif)
 I. Stress and the
Autonomic Nervous System
I. Stress and the
Autonomic Nervous System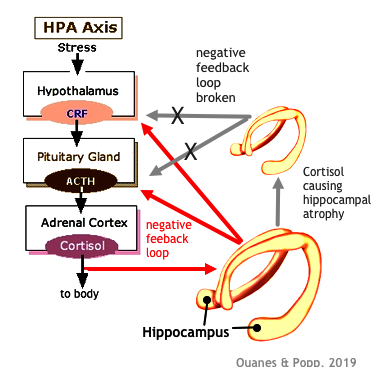 The
hypothalamus sends CRF (corticotropin
releasing factor) to the pituitary gland which
secretes ACTH (adrenocorticotropic hormone)
into the bloodstream which, when it reaches the adrenal
cortex, stimulates the production of cortisol.
When operating normally, elevated levels of cortisol serve
in a negative feedback loop to suppress the further
production of CRF and ACTH. Thus, cortisol inhibits its own
secretion. The hippocampus appears to be a major neural
structure to inhibit the HPA axis; hence, damage to the
hippocampus would be expected to upset the normal
functioning of the axis.
The
hypothalamus sends CRF (corticotropin
releasing factor) to the pituitary gland which
secretes ACTH (adrenocorticotropic hormone)
into the bloodstream which, when it reaches the adrenal
cortex, stimulates the production of cortisol.
When operating normally, elevated levels of cortisol serve
in a negative feedback loop to suppress the further
production of CRF and ACTH. Thus, cortisol inhibits its own
secretion. The hippocampus appears to be a major neural
structure to inhibit the HPA axis; hence, damage to the
hippocampus would be expected to upset the normal
functioning of the axis. 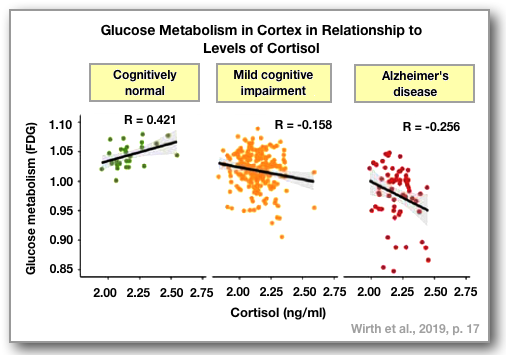 Alzheimer's
Disease (AD)
Alzheimer's
Disease (AD)