|
March 15, 2025 |
PSY 340 Brain and Behavior Class 29: Attack & Escape Behaviors |
|
|
March 15, 2025 |
PSY 340 Brain and Behavior Class 29: Attack & Escape Behaviors |
|
![[Attack...Escape]](../graphics/attack.escape.jpg)
A. Attack Behaviors!
Consider the notion of "aggression." Nations do it when they go to war and humans become aggressive in multiple ways. Chaibi and his colleagues (2023) point out that
Aggression is a social behavior carried out in the context of obtaining or defending limited resources. Aggressive behavior is a biological instinct of humans and animals; it mediates competition for food and habitats (survival instinct), and mating partners (reproductive instinct) and creates stable dominance among social animals’ hierarchies. Aggression represents a normal and even a necessary manifestation as long as it is controlled because it represents the energy that enables the individual to assert and defend himself in relation to others. Although aggression can yield competitive advantages, excessive levels of this behavior are also harmful. They may carry a high risk of injury or death. However, aggression can be considered pathological when it is expressed in exaggerated” (p. 1, citations omitted)As Chaibi et al. (2023) further explain, researchers argue that there are two distinctive subtypes of aggression:
(1) the reactive-impulsive subtype which is strongly allied with negative emotions such as anger and fear and
(2) the proactive-instrumental subtype which tends to be more planned and under control by higher cortical areas of the brain (rather than the limbic system).
The material below reflects and seeks more generally to explain the first subtype: reactive-impulsive aggression.
What are the Environmental and Heredity Factors which have
been shown to lead toward higher levels of aggression and
violence?
Environmental Factors
Genetic factors
No single gene has been found strongly connected to aggressive behavior
> Genetic x Environmental Effects
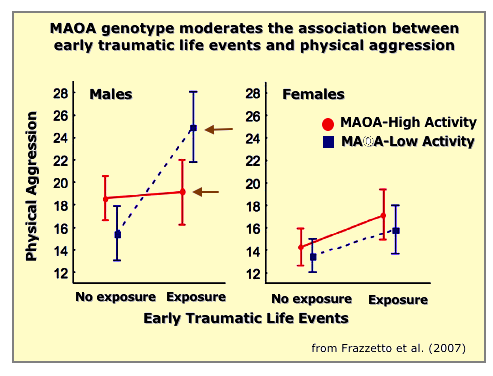
Monoamine oxidase A (MAO-A) is an enzyme which breaks down neurotransmitters dopamine, norepinephrine, & serotonin.
- How much MAO-A is produced is genetically determined with some people showing high MAO-A activity and some showing low MAO-A activity.
Effects of Hormones: Testosterone
- The effects of abuse & maltreatment in children seems to be magnified in those male children with low MAO-A activity. As the figure above shows, when they become adults, they are more likely to be violent or aggressive (Frazzetto et al. 2007).
- In a recent longitudinal study following 2,000 girls into adulthood, Byrd et al. (2019) found that young girls (age 5-12) with the high activity MAO-A gene and subject to childhood maltreatment were much more likely to become more highly emotionally reactive (ER) as teens (ages 13-17). High ER is shown by being touchy, easily annoyed, losing temper, being angry or resentful, taking anger out on others and/or trying to get even with others, In turn, high ER female teens were more likely to show antisocial behavior as early adults (ages 18-21). These behaviors include aggression, impulsivity, and repeatedly doing things that are grounds for legal arrest. See graph of ER in figure on right.
- Male animals across species are more likely to become aggressive against other males
- Men > women: fighting, arrests for violence, verbal rages, etc.
- Highest level of crime occurs in 15 to 25-year-olds, i.e., at the point of the highest level of testosterone
- Note: Testosterone may induce men to be more alert to and/or respond more vigorously to threat
- "Triple-Imbalance Hypothesis"
- Aggression is associated with (1) high testosterone, (2) low cortisol, and (3) low serotonin levels
- May decrease accuracy of identification of facial expressions, e.g., women with temporarily high levels of testosterone become more inaccurate in recognizing facial expressions of anger
Serotonin Synapses & Aggressive Behavior
As the nervous system uses serotonin, it continually reabsorbs or takes back up the serotonin molecules in the synaptic cleft or the serotonin molecules are cut apart by MAO-A. Thus, we can't measure directly how much serotonin an animal's nervous system is using. But, as serotonin is used, it creates a metabolite, 5-HIAA (5-hydroxyindoleacetic acid), which does remain in the synaptic cleft. Hence, measuring how much 5-HIAA exists give us an index of how much "turnover" of serotonin has taken place.Low serotonin turnover = a relative decrease in the amount of serotonin released and taken back into the pre-synaptic neuron.
- Serotonin in Nonhuman Animals
- Linked to aggressive behavior in animals as measured by concentration of 5-HIAA in animals such as mice and hamsters.
- Social isolation of male mouse (over 4 weeks) lowers serotonin turnover & mouse become much more aggressive against other mice.
- Monkeys with low 5-HIAA are much more likely to engage in aggressive behavior than those with higher levels.
- Serotonin in Humans
- Somewhat higher levels of violent behavior in humans is associated with low serotonin turnover, e.g., arson, violent crimes, suicide by violent means or repeated suicide attempts, adolescent and young adult violent crime Why? Serotonin appears to modulate or suppress aggressive impulses.
- Released prisoners with lower levels of serotonin have greater probability of later conviction for violent crime.
- Serotonin is synthesized in the brain from the amino acid tryptophan. In diets low in tryptophan but high in other amino acids (e.g., phenylalanine [in aspartame/NutraSweet®], males tend to become more aggressive a few hours after eating.
- Kamack et al. (2009) found significant reductions in state anger & hostile affect among adults treated with an anti-depressant (citalopram/Celexa®), a drug which increases serotonin turnover.
- By itself, however, low serotonin is not sufficient to make any specific predictions about future behavior of individuals.
Summary: There appears to be some relationship between increased violence and various biological functions (hormones, low serotonin, genetic x environmental interactions). But
B. Escape! Behaviors: Fear and Anxiety
Fear, Anxiety, and the Amygdala
Is there an inborn or unlearned form of fear? Loud noise = startle reflex (present in babies, too) which occurs 2/10th of a second after the sound. Muscles of neck tense up.
- The reaction is greater if one is already tense. Thus, startle reflex is often been used as a gauge of fear or anxiety.
The basic research on the neuroscience of fear has been conducted at the lab of Joseph LeDoux at New York University. He has focused upon the role of the amygdala in the formation of emotional responses. While our text mentions LeDoux earlier in the module, his work is generally ignored in the rest of the module. I intend to focus much more on LeDoux than our text author does.
Amygdala
- Part of the limbic system, the amygdala ("almond" in Latin) is comprised of a collection of a dozen or more nuclei located within/surrounded by the temporal lobe of the brain. It is about an inch inward from each of our ears.
- Amygdala receives information from many sensory & other regions and sends out information to multiple areas as well.
- During the past 20 years, we have learned how central the amygdala is for many aspects of emotion, but particularly regarding the conditions associated with fear and anxiety.
1. Studies in Rats
- Pavlovian Conditioning to Fearful Stimuli
- Conditioned stimulus (CS, e.g. bell) paired with an unconditioned stimulus (UCS, e.g., electrical shock) leads eventually to the development of a conditioned response (CR), i.e., fearfulness.
- Learning takes place via changes of cell connections in the lateral amygdala
- Damage to the amygdala interferes with learning fearfulness
- Implications: Changes in the amygdala are implicated in human anxiety problems such as PTSD, phobias, & panic disorder. It may become overly sensitive to threats in the environment.
2. Studies in Monkeys
Klüver-Bucy Syndrome (Nahm & Pribram, 1998): Damage to the amygdala. This syndrome is found (rarely) in humans. When it is patients with this syndrome have usually experienced either bilateral trauma to the amygdala or been infected with Herpes simplex encephalitis which damaged the amygdala.
- Taming: Placid, loss of aggression
- Psychic Blindness: Inability to recognize objects by sight: No longer fear stimuli such as snakes
- Responsiveness to many small visual cues ("hypermetamorphosis" [Danek, 2007])
- Hyperorality: Examine objects by licking, biting, & chewing
- Hypersexuality
3. Studies in Humans
PET & fMRI: Increased activity in amygdala to pictures of faces showing strong emotions, e.g., fearful, angry, happy
Amygdala will signal the ANS even if shown emotional images too quickly to be consciously comprehended
Originally LeDoux spoke of two "roads" by which we respond to emotional (NOT just FEARFUL) information
- "high road" through the sensory cortex which provides conscious (explicit) recognition after 30-40 ms
- "low road" directly from the thalamus to the amygdala at an unconscious (implicit) level of processing within 12 ms
However, in this model, it looked like the amygdala itself produced the conscious emotion of fear. LeDoux did not mean to suggest this.
Emotion as a Conscious Cognitive State. Since 2016 LeDoux has argued that, in human beings, after receiving information from the sensory systems of the body, the amygdala does not function itself as a "fear" circuit in the brain. It does not produce the emotions of fear or anxiety. Rather, he argues that the amygdala is one of several "defensive survival circuits [that] are evolutionarily wired to detect and respond to innate threats and to respond to novel threats that have been learned about in the past....Defensive survival circuits indirectly contribute to the feeling of fear, but their activity does not constitute fear" (LeDoux & Brown, 2017, p. 2, emphasis added) In LeDoux's argument, both fear (an emotion that responds to a threat NOW) and anxiety (an emotion that responds to a threat in the FUTURE) only become real when we become conscious of the threat and of our unconscious responses.
An alternative and updated diagram of his model is shown below (and based on his August 2017 talk at the APA meeting in DC).
- In this model, the experience of fear (or any other emotion) arises in our conscious working memory from multiple elements that are processed in our working memory at an unconscious level.
Urbach-Wiethe Disease [aka Lipoid proteinosis] (Siebert, Markowitch, & Bartel, 2003)
C. Anxiety DisordersPatients experience degeneration of the amygdala. Siebert et al. report that, compared to normal subjects, these patients had major difficulty in judging all emotions in facial expression, remembering negative and positive pictures, and dealing with an odor-figure association test.
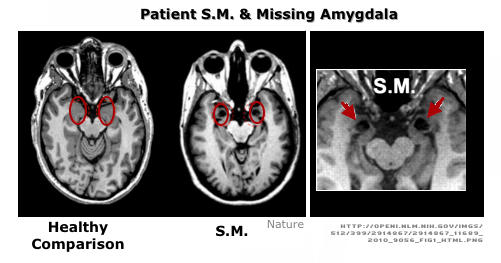
Patient S.M.
(Note this disease has other primary physical symptoms including eyelid beading; thickened woody tongue; hoarseness of voice; skin lesions; seizures)
- Shows no fear of objects and animals (e.g., snakes & spiders) which she claims she fears.
- She has also put herself in dangerous situations, e.g., she has been robbed at gunpoint and physically assaulted a number of times.
- S.M. and other patients with Urbach-Wiether Disease only experienced anxiety and, indeed, a panic attack when exposed to high levels of carbon dioxide (CO2) instead of oxygen. However, even after this experience which was described as terrible, these patients were willing to go through the same experience a week later and did not think about it.
- Damage to amygdala leads to difficulty in recognizing fearful facial expressions and in making social judgments about others' trustworthiness. It appears that such patients focus on the nose and mouth of others rather than either the eyes and, thus, are unable to actually read the actual emotion on the face.
Conclusion: Amygdala seems to be deeply involved in the processing and interpretation of sensory stimuli for its emotional importance or meaning. This means that the amygdala is involved in more than just fear!
Anxiety disorders include generalized anxiety disorder, panic disorder, phobias, and post-traumatic stress disorder (PTSD).
Panic Disorder
- Strong experiences of anxiety
- Often with rapid breathing, increased heart rate, sweating, & trembling, i.e., high sympathetic nervous system arousal
- Patients with panic disorder often feel as if they are about to die though they do not die.
- Women > men; adolescents & young adults > older adults
- Associated with lowered levels of GABA (inhibiting neurotransmitter [see below]) and higher levels of orexin
Post-Traumatic Stress Disorder (PTSD)
- Recollections of event (flashback)
- Nightmares about trauma
- Avoidance of any reminders of the event
- Exaggerated arousal levels (e.g., startle response) to noise and other stimuli
- Occurs at least a month after experience of a trauma in which there was serious threat of injury or death or witnessing other people seriously injured or dead.
Events include soldiering in war, rape, severe automobile accidents, torture, exposure to natural or human-caused disasters (e.g., Oklahoma City Bombing, 9/11, or the Boston Marathon bombing).
While many people have strong stress reactions immediately after a trauma, most do not develop PTSD (that is, <50% exposed to serious trauma actually develop PTSD). Why do some people develop the disorder and others not?
- Individuals with PTSD tend to have a smaller hippocampus than those who do not suffer it. The meaning of this finding in terms of why PTSD develops is not clear
- PTSD patients often show lower than normal levels of cortisol secretion in the days and weeks after the trauma, they may be ill-equipped to handle the damaging effects of stress.
- If the amygdala is damaged, such individuals tend to have no PTSD.
Relief from Anxiety
1. Pharmacological Relief (Medications). The medical treatment of anxiety disorders in the short-term often employs a class of drugs called the benzodiazepines.
- These include diazepam (Valium®), chlordiazepoxide (Librium®), and alprazolam (Xanax®).
Central to the action of the benzodiazepines is the GABA-A receptor complex on the membrane of neurons in the amygdala and hypothalamus (see illustration on right). More specifically, the receptor has five protein subunits.* These subunits each have multiple possible binding sites and the inhibitory neurotransmitter molecule, GABA (gamma-Aminobutyric acid), binds to at least one of these sites. When the GABA molecule attaches to the receptor, a channel opens to let negative chloride ions (Cl-) into the neuron. This serves to hyperpolarize the postsynaptic neuron, i.e., make it less likely to fire, an inhibitory effect.
Benzodiazepines which bind to GABA-nergic sites in the amygdala appear to decrease overall levels of anxiety and fearfulness. How? This may be due to the drug's ability to block the amygdala's processing of fear-inducing information or stimuli.
* Kalat and the literature in general tends to be wrong. During the 1980s and early 1990s, the GABA-A receptor was thought to consist of four subunits. But, more recent research points to five subunits. See <http://www.bioscience.org/1998/v3/d/homanics/3.htm>
- Benzodiazepines seem to suppress various influences that increase the startle reflex
- They also induce sleepiness, block epileptic convulsions, and impair memory
2. Alcohol as an Anxiety Reducer. Another chemical which binds to the GABA-A complex is ethyl alcohol (ethanol). It appears to change the shape of the receptor complex in such a way that GABA molecules themselves bind much more easily. This results in the antianxiety and intoxicating effects of alcohol. Note that these conclusions are tentative and active research into the specific binding sites for ethanol is still ongoing (Harris et al. 2008).
Hoffmann-LaRoche developed a drug, Ro15-4513, which blocks many of the effects of alcohol (it functions as an inverse agonist to GABA). Hence, Ro15-4513 blocks not only the anti-anxiety and other depressant effects of alcohol, but also the motor coordination impairment caused by drinking.
Why is Ro15-4513 not available on the market as a "sobering up" medication? Hoffman-LaRoche realized it was too risky legally:
- People might drive when they were still somewhat impaired. (Note that the law define blood alcohol levels as the standard for DUI.)
- Alcoholics might be driven to drink a great deal more than they do and, without the medication, drink a fatal dose.
3. Relearning to Erase Anxiety
- Anxieties such as phobias tend to be resistant to new learning.
- Children who fear things can sometimes be taught to respond differently by repeated exposure to what they previously feared. Adults are less willing even to undergo such relearning treatment.
- Clinical psychologists have had moderate levels of success in helping those who suffer phobias to relearn less fearful responses.
- Memory Reactivation & Reconsolidation
- A promising approach is the use of propanolol {W}, a beta-blocking drug used for many heart-related conditions, but one which also interferes with protein synthesis in the amygdala. In the treatment of PTSD and other anxiety-related disorders, propanolol has been used with some success by psychiatrists who have patients recall anxiety-related memories. When patients do so under the effects of this drug, they often find significant decreases in their level of fear later on when thinking about those same memories.
- "...after reactivation [previously] consolidated fear memories may return to a transient labile state, requiring a process of restabilization in order to persist [and this finding] offers a window of opportunity for modifying fear memories with amnestic agents...Our research demonstrated that one pill of propranolol (40 mg) administered prior to or after memory reactivation effectively neutralized the fear-conditioned startle response and prevented the return of fear 1 day/month later" Kindt (2018, Abstract & p. 3)
References
Beckley, A. L., Caspi, A., Broadbent, J., Honalee, H., Houts, R. M., Poulton, R., ... Moffitt, T. E. (2018). Association of childhood blood lead levels with criminal offending. JAMA Pediatrics, 172, 166– 173. https://doi.org/10.1001/jamapediatrics.2017.4005
Byrd, A. L., Manuck, S. B. et al (2019) The interaction between monoamine oxidase A (MAOA) and childhood maltreatment as a predictor of personality pathology in females: Emotional reactivity as a potential mediating mechanism. Development and Psychopathology, 31(1), 361-377. https://doi.org/10.1017/S0954579417001900
Carver, C. S., Johnson, S. L., & Joormann, J. (2008). Serotonergic function, two-mode models of self-regulation, and vulnerability to depression: What depression has in common with impulsive aggression. Psychological Bulletin, 134(6), 912-943. https://doi.org/10.1037/a0013740
Chaibi, I., Bouchatta, O., Bennis, M., & Ba-M'hamed, S. (2023). The role of the anterior cingulate cortex in aggression and impulsivity. Behavioral Neuroscience. https://doi.org/10.1037/bne0000552
Danek, A. (2007). ["Hypermetamorphosis". Heinrich Neumann's (1814-1984) legacy]. Nervenzart, 78(3), 342-348. [Abstract. Article in German] https://doi.org/10.1007/s00115-006-2171-2
Frazzetto, G., Di Lorenzo, G., Carola, V., Proietti, L, Sokolowska, E., Siracusano, A, Gross, C., & Troisi, A. (2007). Early trauma and increased risk for physical aggression during adulthood: The moderating role of MAOA genotype. PLoS ONE, 2(5), e486. https://doi.org/10.1371/journal.pone.0000486
Harris, R. A., Trudell, J. R., & Mihic, S. J. (2008, July 15). Ethanol's molecular targets [Abstract]. Science Signaling, 1(28), p. re7. https://doi.org/10.1126/scisignal.128re7
Hayman, L. A., Rexer, J. L., Pavol, M. A., Strite, D., & Meyers, C. A. (1998). Klüver-Bucy syndrome after bilateral selective damage of amygdala and its cortical connections. Journal of Neuropsychiatry and Clinical Neuroscience, 10, 354-358. https://doi.org/10.1176/jnp.10.3.354
Kamarck, T. W., Haskett, R. F., Muldoon, M., Flory, J. D., Anderson, B., Bies, R., Pollock, B., & Manuck, S. B. (2009). Citalopram intervention for hostility: Results of a randomized clinical trial. Journal of Consulting and Clinical Psychology, 77(1), 174-188. Retrieved 03/31/09 from http://0-search.ebscohost.com.library.lemoyne.edu/login.aspx?direct=true&db=psyh&AN=2009-00563-009&site=ehost-live
Kindt, M. (2018). The surprising subtleties of changing fear memory: A challenge for translational science. Philosophical Transactions of the Royal Society-B, 373. https://doi.org/10.1098/rstb.2017.0033
LeDoux, J. (2007, Oct 23). Amygdala. Current Biology, 17(20), R868-R874. https://doi.org/10.1016/j.cub.2007.08.005
LeDoux, J. (2008) Amygdala. Scholarpedia [online] Retrieved 4/8/08 from http://www.scholarpedia.org/article/Amygdala
LeDoux, J., & Brown, R. (2017). A higher-order theory of emotional consciousness. Proceedings of the National Academy of Sciences. https://doi.org/10.1073/pnas.1619316114
Nahm, F. K. D., & Pribram, K. H. (1998). Heinrich Klüver. May 25, 1897-February 8, 1979. Biographical Memoirs, National Academy of Sciences (Vol. 73; pp. 289-305). Washington, DC: National Academy Press. https://doi.org/10.17226/9650
Raine, A. (2019). A neurodevelopmental perspective on male violence. Infant Mental Health Journal, 40, 84-97. https://doi.org/10.1002/imhj.21761
Seo, D., Patrick, C. J., & Kennealy, P. J. (2008). Role of serotonin and dopamine system interactions in the neurobiology of impulsive aggression and its comorbidity with other clinical disorders. Aggression and Violent Behavior, 13(5), 383-395. https://doi.org/10.1016/j.avb.2008.06.003
Siebert, M., Markowitsch, H. J., & Bartel, P. (2003). Amygdala, affect and cognition: Evidence from 10 patients with Urbach-Wiethe disease. Brain, 126(12), 2627-2637. https://doi.org/10.1093/brain/awg271
The first version of this page was posted on April 10, 2005