March 18, 2024
![[Brain Image]](../graphics/head_space.gif)
PSY 340 Brain and Behavior
Class 25: Sex and Hormones
|
March 18, 2024 |
PSY 340 Brain and Behavior Class 25: Sex and Hormones |
|

March 17, 2005: The human X chromosome has been fully decoded and the results published in the journal, Nature. The "X" chromosome, one of the two sex chromosomes, is a DNA sequence of ca. 154-155 million base-pairs coding for ca. 800 proteins in every cell in the human body (vs. ca. 59 million base-pairs in the "Y" chromosome coding for ca. 70 proteins). The sexes are differentiated by the presence of two X chromosomes in females and an X and Y chromosome in males.
A. Becoming
biologically male or female (that is, sexual differentiation)
DifDevelopment in males
- Gonads: the SYR (Sex Region Y) gene on the Y chromosome causes the primitive gonads in males to become testes (sperm-producing organs).
- Testes begin to synthesize testosterone, an androgen hormone. They also produce Müllerian inhibiting hormone (MIH) which cases the Müllerian ducts to disappear. Males produce more androgens than estrogens.
Development in females
- Wolffian ducts develop into the tissues between testes and the penis, i.e., the vas deferens, epididymis, seminal vesicles.
- Gonads become ovaries (egg-producing organs)
- Müllerian ducts develop into the uterus & upper vagina (as long as there is a low level of hormones, especially testosterone).
Hormones: Androgens & Estrogens
- Hormones = chains of amino acids that are secreted in the blood stream and tend to work (see diagram on right) by way of
- Direct effects on the nucleus: the hormone enters the cell, then the nucleus, and then triggers the DNA to produce messenger RNA (mRNA) which causes the synthesis of a new protein, or
- "Second messenger" effects similar to the second messenger effects of some neurotransmitters. The molecules of the hormone attach to receptors of cell membranes which, in turn, release a 2nd messenger inside the cell.
- "Androgens" & "estrogens" are not chemical names, but terms referring to groups of specific steroid hormones (= molecules built of four carbon rings & derived from cholesterol (these hormones are technically lipids [fat-like molecules]))
- Androgens = testosterone (the best known androgen) & other "male" hormones. Levels are higher in males than females. They promote masculine features such as facial hair.
- Estrogens = estradiol (the best known estrogen) & other "female" hormones. Levels are higher in females than males. They produce female features such as breast development.
- Progesterone, a predominantly female hormone, prepares the uterus for implantation of fertilized ovum & promotes pregnancy.
- Cortisol (humans) released by adrenal gland cortex (not the sex glands or gonads, i.e., testes in males and ovaries in females) in response to stress. Promotes breakdown of fats & proteins (including muscle proteins) to be used as energy. Cortisol is neither an androgen nor an estrogen.
- Cortisol is a catabolic steroid because it breaks down muscle proteins (vs. anabolic steroids = testosterone, other androgens, and synthetic molecules based on the androgens are called "anabolic" steroids because they tend to build up (= "ana") muscles. )
B. Organizing
Effects of Sex Hormones
Organizing Effects
Causes permanent structural differences to develop gradually in the body. Usually happens during "sensitive" periods in development of the fetus and newborn infant. However, sex hormones also have organizing effects at puberty, e.g. development of female breasts or male facial hair.
Activating Effects
Causes temporary behavior to occur over seconds, minutes, hours, or days following exposure to hormone(s). Some such effects can be emotional arousal during pregnancy, aggressive behaviors, heightened sexual receptivity, etc.
We have already seen the organizing effect of sex hormones above in the initial development of the sexual organs. What about the continuing organizing effects during pregnancy?
- Male testes secrete testosterone which is converted into dihydrotestosterone (DHT). "DHT is biologically important for sexual differentiation of the male genitalia during embryogenesis, maturation of the penis and scrotum at puberty, growth of facial, body, and pubic hair, and development and maintenance of the prostate gland and seminal vesicles" (Wikipedia). DHT is much stronger in its effects than testosterone by itself.
- Absence of Androgens in Males: Genetic males injected with estrogens experience little effect anatomically. But, the absence of androgens or androgen receptors leads to the development of characteristic female anatomy and female behavior. The absence of androgens may be the result of a genetic mutation, removal of the testes (castration), or exposure to drugs/chemicals during gestation which interfere with androgens, e.g., cocaine, haloperidol (an antipsychotic medication), marijuana, and alcohol.
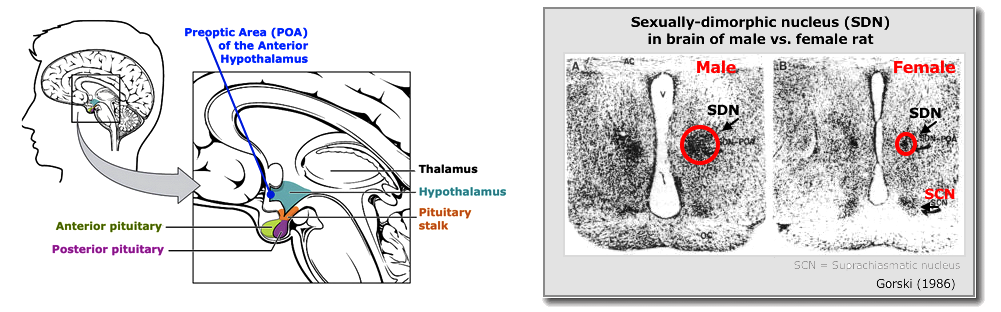
Males
- Sexually dimorphic nucleus (in medial preoptic area of the anterior hypothalamus) has a volume which is between 2.2 and 2.5 times larger in males than females and contains 2.1-2.2 times as many cells in males compared to females (Swaab & Fliers, 1985; Hofman & Swaab, 1989). This area controls male sexual behavior.
- NOTE: "Sexual dimorphic" means that some body organ or tissue is a different size or shape in either males or females.
- Testosterone in male fetus converts into estradiol inside neurons which then "masculinizes" the hypothalamus
Females
- Sexually dimorphic nucleus (in medial preoptic hypothalamus) is smaller in females than males
- Female hypothalamus generates monthly cycle of hormone release (male hypothalamus does not).
- Alpha-fetoprotein in female fetus brain binds to estrogen & prevents it from entering neural cells during sensitive period. Thus, females are not "masculinized" by their own estrogen.
- Range of preferences for play objects among children: boys tend to play with "boy toys" (cars, balls) and girls with "girls toys" (dolls, doll houses). Strong preferences for boy toys by males at 3 years is related to "boy activities" at 13 years and high levels of physical activity at 12 years. Strong preferences for girl toys by females at 3 years is similarly related to higher levels of "girl activities" at 13 years.
- Why?
- Very strong cultural and socialization pressures are certainly there. But....
- Young infants (3-8 months old) show some sexual differences: infant girls prefer to look at dolls rather than trucks (infant boys were equally interested).
- Chemicals in mother's blood during pregnancy may affect fetal brain and subsequent behavior
- Girls whose mothers had higher levels of testosterone in pregnancy showed slightly elevated interest in boys toys at 3.5 years
- Mothers exposed to high level of phthalates {W} (chemicals which inhibit testosterone, used as plasticizers, but also found in perfume, hair sprays, & food packages, etc.) had sons who were less interested in playing with boys' toys at ages 3 to 6 years. (Swan, Liu et al., 2009).
- There is probably some sort of interactive effect of socialization x prenatal environment, especially on boys' behavioral development.
Toxicology & Endocrine Disrupting Chemicals (EDCs)/Hormone Disruptors (not in book). Increasing research evidence has begun to show that a range of environmental toxic chemicals, some of which are labeled as EDCs or "hormone disruptors" are effecting the physical, sexual, and behavioral development of children during both gestation as fetuses as well as in the early childhood years. Among the leading researchers is the epidemiologist, Dr. Shana Swan of Mt. Sinai Hospital in NYC. Her 2009 research cited above of the effects of phthalates on male child behavior was crucial in promoting many other research projects during the past decade.
- In their latest book (2020), Swan & her colleague, Colino, argue that
- Male sexual reproductive capacity in the form of sperm count and sperm concentration have fallen more than 50% across the Western world between 1973 and 2011
- There is a relationship between high prenatal exposure to EDCs and a higher risk of external genital malformation in newborn males (p. 69).
- Exposure to phthalates "can alter male reproductive development in the infant, including the size of the genitals...[and] by early adulthood men whose mothers had higher concentrations of several phthalates during pregnancy have reduced testicular volume , which is associated with lower testicular function." (p. 116)
- In women, higher levels of phthalates have been linked to anovulation (failure to release an egg during a menstrual cycle and polycystic ovary syndrome, a hormonal disorder involving abnormal ovarian function and elevated levels of androgens.
- Daniel et al (2020) found a relationship in the children of mothers in inner city US neighborhoods between maternal exposure to various EDCs (especially phthalates) and higher levels of shyness and anxiety among 7 year old boys and increased impulsivity among girls of the same age.
- A meta-analysis by Lee et al., (2018) found that higher exposure to phthalates is associated with lowered levels of psychomotor development in young children.
C.
Activating Effects of Sex Hormones in Humans
1. Sexual Behavior in Humans
- Activating effects of hormones tend to influence sexual behavior in short time periods (e.g., 15 minutes)
- Oxytocin, a hormone secreted by the pituitary gland, has multiple effects in terms of sexuality and reproduction: (1) stimulating contractions during delivery; (2) stimulating mammary gland to produce milk; and (3) the pleasure and relaxation associated with sexual orgasm. NOTE: Despite what some pop psychology says, OXYTOCIN ≠ A "CUDDLE" OR "LOVE" HORMONE. It has multiple effects (which we will look at later on in a later class) which are sometimes positive and sometimes quite negative in how people interact with one another.
In males
- Testosterone prompts various brain areas (e.g., the medial preoptic area or MPOA) to release dopamine. This release is associated with erections in males and sexual responsiveness in females.
- Serotonin can inhibit dopamine release. Particularly among men, a common side effect of anti-depressant SSRI medications (which increases the amount of serotonin in the brain) involves mild to severe forms of sexual dysfunction. More than 60% of adults treated with SSRIs report lowered levels of sexual interest ("decreased libido") and delayed orgasm. 30% report either an inability to maintain an erection or to reach orgasm. NOTE: In contrast treatment with noradrenergic, dopaminergic, or melatonergic antidepressants is not associated with sexual dysfunction (Montejo, Montejo, & Navarro-Cremades, 2015).
- Sexual excitement is highest when testosterone is highest (ages 15-25 years)
- Decreased testosterone generally decreases sexual activity
- Impotence = inability to have an erection. While this can be due to low levels of testosterone, it is usually related to problems of blood circulation or different medications. Can often be treated by a physician.
- Treatment of sex offenders with medications (e.g., Depo-Provera [progestin or medroxyprogesterone acetate (MPA)]) which radically decrease testosterone has effect: decreases both sexual fantasies and behaviors. However, there are other negative side effects such as weight gain, diabetes, or depression.
In females: the menstrual cycle
Interactive effects of hypothalamus and pituitary gland
- Days 1-5: Menstruation ("menstrual period"): Inner lining of the uterus (the endometrium) partially disintegrates and some blood and other products are discharged.
- Days 5-15: Follicular Phase: Anterior pituitary releases follicle-stimulating hormone (FSH) to promote growth of follicle in ovary. Follicle secretes an increasing amount of estradiol which, in turn, increases production of FSH and luteinizing hormone (LH). Estradiol also causes endometrium to thicken with more blood vessels.
- Days 16-28: Luteal Phase: The FSH & LH causes the follicle to release an ovum (egg), i.e. ovulation. The remnant of the follicle (corpus luteum) releases progesterone which prepares endometrium for implantation of fertilized ovum, prevents development of new follicle, & inhibits uterine contractions.
- If ovum is fertilized, estradiol & progesterone will increase throughout pregnancy.
- Otherwise, if ovum is not fertililzed, LH, FSH, estradiol, & progesterone will all decrease rapidly
- High estradiol and progesterone affect activity of the serotonin-3 receptor (5HT3) leading to nausea in pregnant women.
- Birth Control Pills: Prevent the surge of FSH & LH. Further, estrogen-progesterone pills make it harder for sperm to reach egg or for egg to be implanted.
- Periovulatory period: Midpoint of menstrual cycle when sexual interest & activities increase, perhaps due to effects of higher levels of estrogen.
- Premenstrual Syndrome (PMS & "Premenstrual Dysphoric Syndrome"): A disorder characterized by irritability, anxiety, and depression in the days immediately before the menstrual period. Roughly 85% of menstruating women experience one symptom of PMS and 2-10% of women experience serious symptoms which interfere with work, school, etc. (Dickerson et al., 2003) [Not in book]
Sex Hormones & Nonsexual Characteristics
- Beware of arguments that the brains of men and women are extremely different. They simply are not. We covered this topic earlier in the semester.
- Specific brain differences include
- "Males [have] higher cortical and sub-cortical volumes, cortical surface areas, and white matter diffusion directionality; females [have] thicker cortices and higher white matter tract complexity." (Ritchie et al, 2018, Abstract)
- There are some small to moderate differences between males and females in the functional connections between parts of the brain in the resting state, i.e., when individuals are not doing any specific mental task: "Connectivity [in resting state fMRI] between sensorimotor, visual, and rostral lateral prefrontal areas was stronger in males than females (see orange cluster of brain regions in Figure 4A [see 4B, too]), whereas connectivity within the default mode network (DMN; red cluster of regions in Figure 4A [see 4C, too]) was stronger in females than males." (Ritchie et al., 2018, p. 2967; see figure above)
- However, as Joel et al. (2015) argue in a widely-cited study: "Although there are sex/gender differences in brain and behavior, humans and human brains are comprised of unique “mosaics” of features, some more common in females compared with males, some more common in males compared with females, and some common in both females and males. Our results demonstrate that regardless of the cause of observed sex/gender differences in brain and behavior (nature or nurture), human brains cannot be categorized into two distinct classes: male brain/female brain" (p. 15468; emphasis added)
Dr. Janet Shibley Hyde is professor of psychology and women's studies at the University of Wisconsin-Madison. Her "meta-analyses of the current body of research on gender difference cast aside both the difference and deficit models — the idea that women just aren’t quite as capable as men overall — in support of what she has titled the gender similarities hypothesis: the theory that “men and women are very similar on most (not all) psychological variables.” Or, to put it even more simply: “women are from Earth and men are from Earth.” (Armstrong, 2019) [in contrast to the pop psychology book by John Grey in 1992 called Men Are From Mars; Women Are From Venus {W}, a volume which has been widely criticized by research psychologists.]
- Recognition of Facial Expression of Emotion. Females > males. Under experimental administration of testosterone, females become less accurate in identifying anger. This suggests that testosterone interferes with processing emotional expression.
1. Behavior in Mammals
- Among many mammals, parental behavior appears to depend both upon hormones and upon other factors.
- An increase in oxytocin and prolactin by the day of delivery is necessary for the onset of maternal behavior in female rats.
- Damage to the medial preoptic area impairs parental behavior in rats.
- Later stages of maternal behavior are not dependent on hormones, but upon the mother's experience interacting with offspring/pups.
- In male rats, testosterone levels drops after the delivery of their pups and prolactin levels increase.
2. Human Parental Caregiving (this is not in text but required)
- No obvious or dependable parallels between parenting in other mammals and in humans.
- Humans give birth to semiprecocial offspring (= mostly dependent on parent but still capable of some expressive behaviors, e.g., crying, eyes open). Other animals give birth to precocial offspring who can cope with the environment well very soon after birth. "Precocial species are those in which the young are relatively mature and mobile from the moment of birth or hatching." {W} Precocial young are born with eyes open, able to walk, feed themselves and can keep themselves warm. Examples of precocial animals would include domestic chickens, Canada geese, turkeys, mountain goats and horses. The words "precocial" and "precocious" come from the same root meaning "early maturing" The opposite to precocial in zoology (animal studies) is altricial in which the newly-born animal is completely helpless, born with its eyes closed, and utterly dependent on the parent to survive.
- Fathers are more affectionate & attentive to infants if they have lowered testosterone levels.
Human Parent-Infant Caregiving (Feldman, 2007, 2015, 2016)
- Among humans the bond between parent and infant forms the basis of the family and, from that bond, the child is molded or shaped to enter into the cultural world of that family.
- Usually, under the early influence of oxytocin there is a rapid bond that forms between mother and child as they engage in close physical and affective (emotional) contact. As the mother-child bond develops, it becomes much less dependent on any hormonal influences.
- A predominant behavioral pattern between mother and infant is called "synchrony" ("syn"= together; "chronos" = time, therefore, "at the same time"). This means that, in their face-to-face encounters, both mothers and babies exchange a wide and coordinated range of affective and other social cues. These may include touching, gazing, smiling, and a kind of high-pitched speech called "motherese". As Feldman (2015) describes, "social synchrony ... triggers biological synchrony between the parent’s and child’s physiology. During synchronous moments, the parent’s and infant’s heart rhythms and oxytocin levels synchronize" (p. 394).
- In contrast to other animals, human parents are high influenced by human culture which shapes the goals of the parents and, often, the ways in which parents interact with their offspring.
- The ability of mothers to respond to their newborn infants involves sensitivity to and appropriate responsiveness to the various cues and signals that an infant gives off. There are multiple, interacting systems in the brain which are engaged in maternal responses to babies (Kim et al. 2016). These include
- reward/motivation brain systems in the neocortex and amygdala dependent upon dopamine and oxytocin
- emotional regulation systems in the brain which allow mothers to recognize and respond to distress in their infants
- systems that allow parental empathy ("appropriate perception, experience, and response to another's emotion" p. 115)
- executive control systems (including attention, inhibitory control, working memory, flexibility in task-switching) permit mothers to deal with infants' needs more effectively.
- Difficulties in sensitivity and responsiveness by new mothers can arise from multiple sources including (1) the mother's own experience of maternal warmth as a child, (2) any affective disorders like depression before giving birth, and (3) postpartum maternal psychopathology (depression, substance abuse, post-traumatic stress disorder).
References
Armstrong, K. (2019, February). Janet Shibley Hyde sinks stereotypes with data. APS Observer. Retrieved from https://www.psychologicalscience.org/observer/janet-shibley-hyde-sinks-stereotypes-with-data
Daniel, S., Balalian, A. A., Insel, B. J. et al. (2020). Prenatal and early childhood exposure to phthalates and childhood behavior at age 7 years. Environment International, 143. https://doi.org/10.1016/j.envint.2020.105894
Dickerson, L. M., Mazyck, P. J., & Hunter, M. H. (2003, April 15). Premenstrual syndrome [Online]. American Family Physician, 67, 1743-1752.
Feldman, R. (2007). Parent-infant synchrony: Biological foundations and developmental options. Current Directions in Psychological Science, 16(6), 340-345. https://doi.org/10.1111/j.1467-8721.2007.00532.x
Feldman, R. (2015). The adaptive parental brain: Implications for children’s social development. Trends in Neurosciences, 38(6), 387-399. https://doi.org/10.1016/j.tins.2015.04.004
Feldman, R. (2016). The neurobiology of mammalian parenting and the biosocial context of human caregiving. Hormones and Behavior, 77, 3-17. https://10.1016/j.yhbeh.2015.10.001
Gorski, R. (1986). Sexual differentiation of the brain: A model for drug-induced alterations of the reproductive system. Environmental Health Perspectives, 70, 163-175. https://doi.org/10.1289/ehp.8670163
Hofman, M. A., & Swaab, D. F. (1989). The sexually dimorphic nucleus of the preoptic area in the human brain: a comparative morphometric study. Journal of Anatomy, 164, 55-72. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1256598/
Joel, D., et al (2015) Sex beyond the genitalia: The human brain mosaic. PNAS, 112(50), 15468-15473. https://doi.org/10.1073/pnas.1509654112
Kim, P., Strathearn, L, & Swain, J. E. (2016) The maternal brain and its plasticity in humans. Hormones and Behavior, 77, 113-123. https://doi.org/10.1016/j.yhbeh.2015.08.001
Lee, D.-W., Kim, M.-S., Lim, Y.-H, Lee, N., & Hong, Y.-C. (2018) Prenatal and postnatal exposure to di-(2-ethylhexyl) phthalate and neurodevelopmental outcomes: A systematic review and meta-analysis. Environmental Research, 167, 588-566. https://doi.org/10.1016/j.envres.2018.08.023
Lilienfeld, S. O., Sauvigné, K. C., Lynn, S. J., Cautlin, R. L., Latzman, R. D., & Waldman, I D. (2015). Fifty psychological and psychiatric terms to avoid: A list of inaccurate, misleading, misued, ambiguous, and logically confused words and phrases. Frontiers in Psychology, 6, Artlcle 1100. https://doi.org/10.3389/fpsyg.2015.01100
Kimura, D. (2002, April 1). Sex differences in the brain [Online] Scientific American. https://www.academia.edu/17891561/2002Scientific_American_Sex_Differences_In_The_Brain
Montejo, A. L., Montejo, L., & Navarro-Cremades, F. (2015). Sexual side-effects of antidepressant and antipsychotic drugs. Current Opinion in Psychiatry, 28, 418-423. https://doi.org/10.1097/YCO.0000000000000198
Ritchie, S. J., Cox, S. R., ... & Deary, I. J. (2018). Sex differences in the adult human brain: Evidence from 5,216 UK Biobank participants. Cerebral Cortex, 28(8), 2959-2975. https://doi.org/10.1093/cercor/bhy109
Swaab, D. F., & Fliers, E. (1985). A sexually dimorphic nucleus in the human brain. Science, 228(4703), 1112-1115. https://dx.doi.org/10.1126/science.3992248
Swan, S. H. & Colino, S. (2020). Count down: How our modern world is altering male and female reproductive development, threatening sperm counts, and imperiling the future of the human race. New York, NY: Scribner.
Swan, S. H., Liu, F., et al. (2009) Prenatal phthalate exposure and reduced masculine play in boys. International Journal of Andrology, 33(2), 259-269. https://10.1111/j.1365-2605.2009.01019.x
The first version of this page was posted on March 20, 2005.