Feb 15, 2025
![[Brain Image]](../graphics/head_space.gif)
PSY/BSC 340 Brain and Behavior
Class 17: Plasticity after Brain Damage
|
Feb 15, 2025 |
PSY/BSC 340 Brain and Behavior Class 17: Plasticity after Brain Damage |
|
Plasticity After Brain Damage: How does the brain get damaged and long-term outcomes
Plastic => Latin, plasticus ="of molding," from Greek plastikos, from plassein = "to mold, form" How much can the brain be molded or formed (or changed or adapt) after it has been damage?
I. Brain Damage and Short-term Recovery
A. How is the brain damaged?
- Illness
- Vascular Disorders: Stroke
- Tumors
- Infection
- Bacterial, e.g., bacterial meningitis: very serious threat for college students
- Viral, e.g., viral meningitis
- Injury
- Traumatic Head Injury
- Open Head Injury, e.g., bullet wound
- Closed Head Injury, e.g., car accident, bicycle accident, blow to the head (see below)
- Epilepsy
- Drugs-Alcohol-Chemical Toxicity
- Genetics & Inherited Degenerative Diseases
- Parkinson's Disease
Huntington's Chorea
- Unknown Origin: Alzheimer's Disease & Other Dementing Illnesses (e.g. frontotemporal deterioration [FTD])
B. Specific Types of Damage
1. Closed Head Injury = sharp blow to the head which does not puncture the brain
- Rotational forces leading to
- shearing
- twisting
- Coup-contrecoup leading to
- contusion (damage to tissue)
- swelling (edema)
- hemorrhage/blood clots
This is the most common type of head injury in younger people. Caused by car & motor cycle accidents, falls, etc. While 80-85% of closed head injuries are mild, about 5-10% are quite severe and lead to long-term problems.
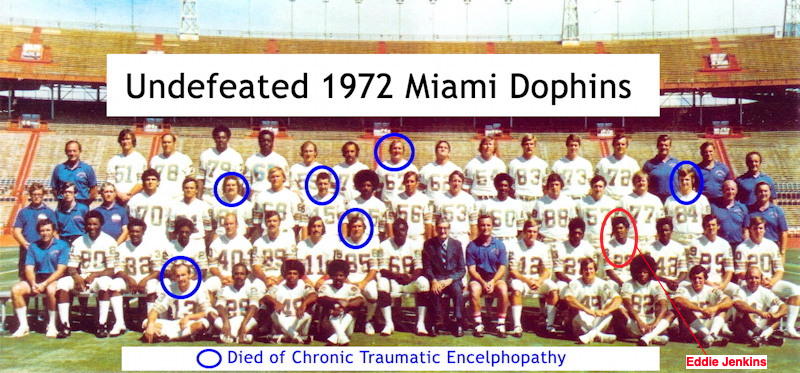
- Rising problem of Chronic Traumatic Encephalopathy (CTE) in football players and other sports. "Chronic traumatic encephalopathy (CTE) is a neurodegenerative disease found in people who have had multiple head injuries. It is most commonly found in those who have participated in contact sports on a regular basis." [Wikipedia]

2. Stroke (cerebrovascular accident [CVA]) = temporary or permanent loss of blood flow to a brain area (Tan & Lui, 2022)
A. Two Types of Strokes
- Ischemic: obstruction, blood clot, or temporary narrowing of blood vessel closes off blood supply [ischemia]. Damage comes from loss of oxygen and glucose. Around 87% of all strokes in the United States are ischemic.
- Hemorrhagic: artery or other blood vessel ruptures spilling blood into the brain tissue & surrounding area [hemorrhage]. Damage directly occurs from effects of blood & excess oxygen, calcium, and other waste products. Around 13% of all strokes in the United States are hemorrhagic.
- Severe dangers comes from edema (= swelling of brain tissue) & excess of sodium (NA+) & other ions which the Na-K pump can't handle.
B. Reducing Harm from a Stroke
- Thrombolytic Therapy using Tissue Plasminogen Activator (tPA): breaks up blood clots in an ischemic stroke. Should be used within 4.5 hours of initial stroke. HOWEVER, tPA is counter-indicated for hemorrhagic stroke. And, this treatment helps a limited number of patients because of the time limitation.
- Mechanical Thrombectomy = a surgical procedure used to remove blood clots from arteries and veins [that is, in an ischemic stroke] in which the surgeon inserts a catheter into a patient’s blood vessel to remove the blockage and restore blood flow to the affected area. This procedure can be used between 6 and 24 hours since the beginning of the stroke.
==> Unfortunately these two approaches above are helpful in only a small percentage of ischemic stroke.
- Therapeutic Hypothermia (TH) = Cooling brain (from 98.6 degrees to 91-96 degrees F). If begun within 2 hours after the event, and continued for at least 1-3 days, the survival and long-term neurological outcome appears improved for both new-born infants who suffer a stroke and for others who have had a sudden heart attack depriving the brain of blood/oxygen. (Chiu et al, 2023, You et al, 2022). The effectiveness of TH in adults who have suffered a stroke is far less certain in the research literature (Whitelaw & Thoresen, 2023)
- Experimental work on glutamate receptor blockers; Early results with these drugs have been both disappointing and shown variable outcomes. More recent work is beginning to formulate an approach that might have beneficial effects on preventing neural cell death (Ge et al., 2020; Frank et al., 2022).
II. Later Mechanisms of Recovery
A. Increased Brain Stimulation
Diaschisis (Greek, = "shocked throughout")
decreased activity of surviving neurons throughout the brain after damage to other neurons.
- More distant neurons (not damaged) may no longer receive stimulation from areas of damage. This leads to overall decreased activity in nervous system.
- Recovery from stroke often requires increased stimulation from the contralateral side of the body.
- Tranquilizers impair recovery
B. Regrowth of Axons
- Crushed or damaged axons in the PNS grow back at a rate of 1 mm per day
- Damaged axons in the CNS only grow about 1 mm at most
- In spinal cord, damage creates scar tissue & synthesizes a chemical that stops axon growth
- Myelin in the CNS secretes a protein to inhibit axon growth (in the PNS this is not true)
- We look for the day when spinal cords might be able to regrow adequately to restore functions
- Research with neurotrophins and other substances with laboratory animals has shown some promise for promoting regrowth of axons.
C. Axon Sprouting
- After a connecting axon is damaged, neurons to which they were connected secrete neurotrophins. This induces other, undamaged axons to form new branches. These are called collateral sprouts. These fill in vacancies at synapses.
- The effects of collateral sprouts can be helpful or harmful. Sometimes these sprouts replace lost connections and restore functioning, e.g., in the hippocampus. But, sprouts in the visual cortex might cause additional faulty vision, e.g., making an object appear in the visual field that is not really there.
D. Denervation Supersensitivity
- If a postsynaptic cell loses a connection to other neurons, it becomes more sensitive to the neurotransmitters that it does receive. It builds additional receptors which make use of whatever neurotransmitter is available.
- The heightened sensitivity to a neurotransmitter after the destruction of synapsing axons is called denervation supersensitivity.
- This phenomenon serves an adaptive function by allowing neurons or other cells to act even with reduced stimulation. Hence, despite the loss of many axons, individuals may still be able to retain functioning nonetheless.
E. Reorganized Sensory Representations and the Phantom Limb
Phantom Limb phenomenon = The continuing sensation of an amputated body part
- Range of experience: tingling ==> intense pain
- What is happening?
- Representation shifts in the somatosensory strip
- Transplants and artificial limbs can lead to a lessening or elimination of phantom limb pain
- Major investigator & theorist of this phenomenon is Vilayanur Ramachandran, MD, Ph.D., (UC San Diego; homepage)
- Gave the 2003 Reith Lectures on The Emerging Mind for the BBC
- As we previously saw, he is the major innovator in the use of mirrors to treat phantom limb pain
F. Learned Adjustments in Behavior
- Deafferented limbs: loss of sensory (afferent) input does not mean that the limb cannot be moved. Indeed, when forced to do so, limbs can be used.
- Rehabilitation by physical and occupational therapists often puts person in restrained mode to force the use of neglected limbs/muscles. Note that this is difficult and tiring. Individuals in rehabilitation have significant problems with the use of alcohol, stress, or efforts that intact individuals would not have.
Clinical Neuropsychology
If you find the material for this class particularly interesting, you should know that some of it comes from a field called "clinical neuropsychology" -- the study of the behavior of brains that are damaged. I will next teach my PSY 448 course on this topic in the Fall, 2025.
Students who might want to study clinical neuropsychology as graduate students can check out the webpages of the American Psychological Association's Division 40 Clinical Neuropsychology for information on graduate programs, etc. Similarly, you might look over the student materials at the American Academy of Clinical Neuropsychology (whose incoming President-Elect, Dr. Dominic Carone, is a Le Moyne College graduate!)
References
Berman, M. R. (2023, February 23). Bruce Willis’ frontotemporal dementia. MedPage Today [Internet]. https://www.medpagetoday.com/popmedicine/celebritydiagnosis/103236
Chiu, P.-Y., Chung, C.-C., Tu, Y.-K. et al (2023). Therapeutic hypothermia in patients after cardiac arrest: A systematic review and meta-analysis of randomized controlled trials. American Journal of Emergency Medicine, 71, 182-189 . https://doi.org/10.1016/j.ajem.2023.06.040
Frank, D., Zlotnik, A., Boyko, M., & Gruenbaun, B. F. (2022). The development of novel drug treatments for stroke patients: A review. International Journal of Molecular Sciences, 23, 5796. https://doi.org/10.3390/ijms23105796
Ge, Y., et al (2020) NMDARs in cell survival and death: Implications in stroke pathogenesis and treatment. Trends in Molecular Medicine, 26(6). https://doi.org/10.1016/j.molmed.2020.03.001
Tadi P, & Lui F. [2022, Nov. 4] Acute stroke. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK535369/
Vicente-Acosta, A., Ceprian, M., Sobrino, P., Pazos, M. R., & Loría, F. (2022). Cannabinoids as glial cell modulators in ischemic stroke: Implications for neuroprotection. Frontiers in Pharmacology, 13. https://doi.org/10.3389/fphar.2022.888222
Whitelaw, A., & Thoresen, M. (2023) Therapeutic hypothermia for hypoxic–ischemic brain injury is more effective in newborn infants than in older patients: Review and hypotheses. Therapeutic Hypothermia and Temperature Management, 13(4). https://doi.org/10.1089/ther.2023.0050
You, J. S., Kim, J. Y., & Yenari, M. A. (2022) Therapeutic hypothermia for stroke: Unique challenges at the bedside. Frontiers in Neurology, 13. https://doi.org/10.3389/fneur.2022.951586
The first version of this page was posted on February 18, 2005.