January 25, 2025
![[head]](../graphics/head.gif)
PSY 340 Brain and Behavior
Class 09: Substance Abuse and Addiction
|
January 25, 2025 |
PSY 340 Brain and Behavior Class 09: Substance Abuse and Addiction |
|
- Jimi Hendrix (1942-1970). Musician. Alcohol & barbiturate overdose. Inhalation of vomit.
- Heath Ledger (1979-2008). Actor. Accidental. "died of the combined effects of five (5) prescription & one (1) over-the-counter medications: oxycodone, hydrocodone, diazepam, temazepam, alprazolam, and doxylamine (Unisom®)
- Michael Jackson (1958-2009). Singer. Homicide. MD administration of propofol, lorazepam, diazepam, & midazolam.
- Whitney Houston (1963-2012). Singer, actress. Accidental drowning. Cocaine + Benadryl, Flexeril, Xanax.
- Philip Seymour Hoffman (1967-2014). Actor. Heroin overdose.
- Prince Rogers Nelson (1958-2016) Accidental overdose of fentanyl
- Lil Peep (Gustav Ahr; 1996-2017). Rapper and singer. Multiple Xanax (alprozalam) pills. Blood showed traces of cannabis, cocaine, tramadol, hydrocodone, hydromorphone, oxycodone, & oxymorphon.
- Tom Petty (1950-2017) Singer, songwriter, musician. Accidental overdose of opioids including fentanyl & oxycocode, two sedatives, and an antidepressant.
- Mac Miller (1992-2018). Rapper, songwriter. Accidental overdose of fentanyl, cocaine & alcohol
- DMX (1970-2021). Rapper. Drug-induced (cocaine) heart attack.
- Taylor Hawkins (1972-2022). Drummer for Foo Fighters. Apparent heart disease/attack. Multiple drugs found in his system at the time of death included opioids, benzodiazepines, tricyclic antidepressants, and THC (active ingredient in marijuana, see below).
I.
Drug Mechanisms
Types of Drug Effects
- Antagonist: a drug that blocks the effect of a neurotransmitter
- Agonist: a drug that increases or mimics the effects of a neurotransmitter
- Some drugs are mixed agonist-antagonists, that is, they prompt some behaviors of the neurotransmitter they mimic while blocking other behaviors.
Other Qualities of Drugs
- Affinity: tendency of a drug to bind to a receptor (strong to weak)
- Efficacy: tendency of a drug to activate a receptor (high to low)
- Note that some drugs may bind to a receptor but do nothing else. This drug can be described as having a high affinity, but low efficacy.
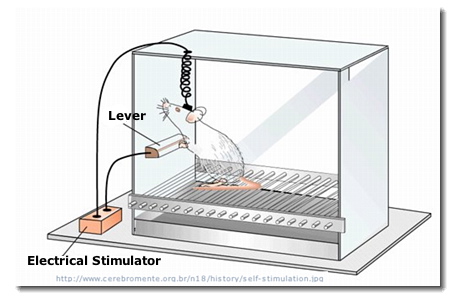 James Olds & Peter Milner
(1954) found areas in rat's brain which leads to continual self-stimulation.
Pressing the lever in the experimental situation (see diagram on
left) appears to have been very reinforcing for the rats. All of
these areas associated with reinforcement
James Olds & Peter Milner
(1954) found areas in rat's brain which leads to continual self-stimulation.
Pressing the lever in the experimental situation (see diagram on
left) appears to have been very reinforcing for the rats. All of
these areas associated with reinforcement 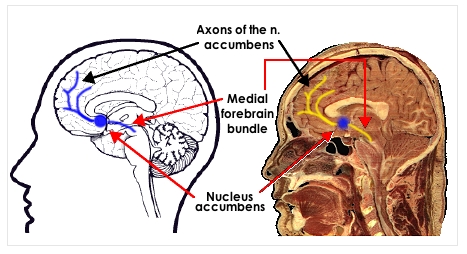 eventually were seen to increase the release of
dopamine in the nucleus accumbens (see diagram).
eventually were seen to increase the release of
dopamine in the nucleus accumbens (see diagram). 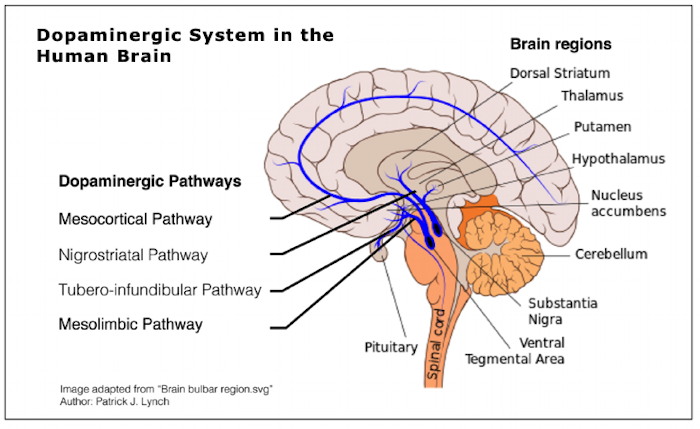 Research in the last several decades points
to dopamine as involved in more than the reinforcement Olds
& Milner found in 1954. As the National Institute of Drug
Abuse (NIDA, 2020) reported "The neurotransmitter dopamine helps
people remember the pleasurable effects of drugs and reinforces
the desire to seek them out again, making it centrally involved
in addiction.
Research in the last several decades points
to dopamine as involved in more than the reinforcement Olds
& Milner found in 1954. As the National Institute of Drug
Abuse (NIDA, 2020) reported "The neurotransmitter dopamine helps
people remember the pleasurable effects of drugs and reinforces
the desire to seek them out again, making it centrally involved
in addiction. Though these seem
similar, they are not. As Berridge & Robinson (2016)
note:
Rewards are both “liked” and “wanted,” and those 2 words seem almost interchangeable. However, the brain circuitry that mediates the psychological process of “wanting” a particular reward is dissociable from circuitry that mediates the degree to which it is “liked.” Incentive salience or “wanting,” a form of motivation, is generated by large and robust neural systems that include mesolimbic dopamine. By comparison, “liking,” or the actual pleasurable impact of reward consumption, is mediated by smaller and fragile neural systems, and is not dependent on dopamine. [Abstract]
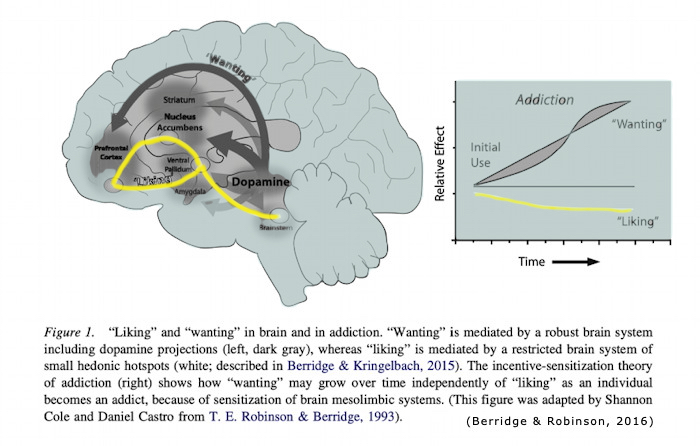
In this theory,
dopamine is NOT associated directly with liking or pleasure,
but it IS centrally involved in making an individual desire or
want something intensely. "Liking" comes from a variety of
"hot spots" in the brain (NOT the nucleus accumbens) which do
respond to the molecules of a substance which is addictive
(see diagram to right).
Recent studies
suggest that dopamine and the nucleus accumbens actually play
an important role in attention-getting or arousal.
Addiction seems to have a quality of demanding attention
(increasing your craving or wanting something
= salience) and this may be the link (rather than via
the "pleasure" effects of chemicals)
Note that individuals
with addiction show an overwhelming urge to get the drug even
after the pleasure has stopped.
Over time as
addiction develops, the enjoyable effects of the drug tends to
decrease. This is called tolerance. The addicted
individual must use more of the drug to achieve the same level
of reward. A great deal of the phenomenon of tolerance
involves learning, i.e., conditioned and strengthening
associations between the setting and mechanisms of drug
ingestion and the body's response to the drug. Indeed,
repeated exposure to typical drug use settings without actual
drug use will weaken the association.
However, whenever an
addict is exposed to settings in which he/she has typically
used the drug, there can be a very strong reaction even if no
drug is ingested. This reaction is called withdrawal. Symptoms
of withdrawal include anxiety, sweating, vomiting, and
diarrhea for opioids and tiredness, shaking,
sweating, nausea, convulsions, and hallucinations
for chronic alcohol abuse.
Is all drug use in
chronic drug users an attempt to avoid withdrawal symptoms?
Some Drugs of Abuse (not in
book)
1. Stimulant drugs
(e.g., amphetamines, cocaine, etc.)
a. Amphetamine increases dopamine (DA) release from presynaptic terminals and also reverses the direction of the dopamine transporter (reuptake gate) which makes more DA available.
b. Cocaine ("coke") blocks the reuptake of DA, NE, and serotonin at the synapse. The behavioral effects of cocaine are believed to be mediated primarily by dopamine and secondarily by serotonin.
c. The effects of amphetamine and cocaine are both short-lived, because of the depletion of dopamine stores and tolerance.
d. Methylphenidate (Ritalin®): Stimulant currently prescribed for Attention Deficit Disorder (ADD); works like cocaine by blocking reuptake of dopamine at presynaptic terminals. The effects of methylphenidate are much longer lasting and less intense as compared to cocaine.
--> the use of Ritalin® when used as prescribed does not lead to the use of other drugs in later life.
e. MDMA (methylenedioxymethamphetamine or "Ecstasy") at low doses is a stimulant which increases the levels of dopamine. At higher doses it releases serotonin and may have hallucinogenic effects.
![[Don't
Smoke]](../graphics/no.smoking.jpg) 2. Nicotine
2. NicotineNicotinic receptor stimulation leads to increased responsiveness and activity levels in novel settings
Common opiates include
 morphine
morphine  heroin
heroin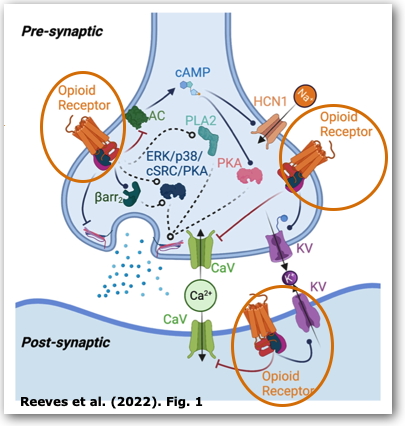 Opioid Receptors (=
inhibitory G protein-coupled receptors)
Opioid Receptors (=
inhibitory G protein-coupled receptors)
4. Marijuana
5. Alcohol and Alcoholism
![[Effects
of ETOH on body]](../graphics/etoh.jpg)
A. Alcoholism or alcohol dependence: A common type of substance abuse that produces significant harm to people's lives, and those people often find themselves continuing to drink in excess even after deciding to quit or reduce their drinking.
B. Alcohol (ethanol, ETOH): Inhibits Na+ ion flow across the neuron membrane; decreases serotonin activity, facilitates transmission at the GABAA receptor, blocks glutamate receptors, and increases dopamine activity. Thus, alcohol is mostly an INHIBITORY substance.
C. There have been multiple attempts to classify subtypes of alcoholism. One important effort was undertaken by the researcher Robert Cloninger on the basis of adoption studies among Scandinavian alcoholics. The two subtypes in his classification scheme (Oreland et al, 2017) are:
• Type I Alcoholism: This type of alcoholism is less dependent on genetic factors and has a late onset, that is, it develops gradually over years (> 25 years old). It tends to affect men and women equally, and is generally less severe. It is often the result of years of leading a stressful life and using alcohol to cope with the stress.
• Type II Alcoholism: This type of alcoholism has a strong genetic basis and a rapid and early onset (< 25 years old), affects men primarily, is more severe, is associated with the use or abuse of other substances, and reflects others social problems, e.g., a family history of alcoholism, depression, and antisocial or criminal behavior (fighting & arrests)
D. Predispositions for Alcoholism & Substance Abuse
i. Alcoholism: Tends to be more likely among those who, as children, were described as impulsive, risk-taking, easily bored, sensation-seeking, & outgoing.
Associated with genes causing
- "long form" dopamine type 4 receptors: these receptors tend to be less sensitive to ETOH and, thus, people tend to consume more, and
- more active form of COMT (enzyme breading down DA) leading to lower levels of reinforcement & higher levels of impulsiveness.
ii. Among sons of alcoholics, alcoholism is associated with
- less than average intoxication after drinking a moderate amount of alcohol.
- experiencing more than average relief from tension after drinking alcohol.
- having a smaller than normal amygdala in the right hemisphere
iii. Genetic influences on drug abuse
- Strong evidence for polygenetic influences on alcoholism, cocaine use, and some other drugs. NO individual genes, but many genes contribute toward this vulnerability.
- The same genes that create an addiction vulnerability to substances like alcohol are associated with bipolar disorder, conduct disorders, and antisocial personality disorder.
iv. Environmental Influences
- Mothers who drink alcohol during pregnancy have children with a greater risk of alcoholism in later life
- Children with a variant gene for a less sensitive GABA receptor tend to have impulse control problems (including drug use) unless they grow up in families which clear parental supervision.
- Medications to Combat Opioid Abuse
- The most effective medical treatment for opioid (heroin, etc.) abuse in patients who have failed to "kick their habit" by more traditional treatment methods is the use of suboxone or methadone.
- Suboxone is a prescription medicine that contains the active ingredients buprenorphine (an opioid which has a slow onset, has a mild effect, and is very long acting with a half-life of 24 to 60 hours) and naloxone (a drug that blocks the effects of opioids). Suboxone is very effective in preventing accidental overdoses which lead to death.
- Methadone as noted above is a synthetic ("man made") opioid which is taken orally once a day. It does not lead to heroin "highs" but does relieve the cravings for heroin. Methadone is usually used with individuals who have failed multiple times in other treatment approaches. In the form of methadone maintenance therapy, it is taken for long periods of time (even for a lifetime) as a way of preventing the use of heroin. In methadone reduction therapy, it is taken over a period of time, but tapered down until the individual no longer feels the need to consume an opioid.
- Note that our textbook says, "these drugs do not end the addiction. They merely satisfy the craving in a less dangerous way" (p. 472). I inserted a bold-faced italics for the word "merely" because it can be interpreted as a moral judgment by the author and, certainly, many others object to "substituting" one opioid for another since, in some fashion or another, the addict is not only medically-impaired, but considered to be a moral failure. As Maia Szalavitz and others point out, however, physicians and other treatment givers should not be in the business of condemning people, but saving their lives. When the alternative to suboxone and methadone is so frequently death, it would seem that keeping people alive ought to be the principal goal of health care providers.
ReferencesActive/Lethal Dose Ratio and Dependence Potential of Psychoactive Drugs. Data source: Gable, R. S. (2006). Acute toxicity of drugs versus regulatory status. In J. M. Fish (Ed.),Drugs and Society: U.S. Public Policy, pp.149-162, Lanham, MD: Rowman & Littlefield Publishers. Image retrieved from http://en.wikipedia.org/wiki/File:Drug_danger_and_dependence.svg
Berridge, K. C., & Robinson, T. E. (2016). Liking, wanting, and the incentive-sensitization theory of addiction. American Psychologist, 71(8), 670-679. https://dx.doi.org/10.1037/amp0000059
Case, A., & Deaton, A. (2017, Spring). Mortality and morbidity in the 21st century (Brookings Papers on Economic Activity). Washington, DC: Brookings Institution. Retrieved from https://www.brookings.edu/wp-content/uploads/2017/08/casetextsp17bpea.pdf
NIDA (2020, March 27). Dopamine neurons signal rich information about unexpected events. https://www.drugabuse.gov/news-events/science-highlight/dopamine-neurons-signal-rich-information-about-unexpected-events
Oreland, L., Lagravinese, G., et al (2017). Personality as an intermediate phenotype for genetic dissection of alcohol use disorder. Journal of Neural Transmission. doi:10.1007/s00702-016-1672-9
Reeves, K. C., Shan, N., Muñoz, B., & Atwood, B. K. (2022). Opioid receptor-mediated regulation of neurotransmission in the brain. Frontiers in Molecular Neuroscience, 15. https://doi.org/10.3389/fnmol.2022.919773
Torregrossa, M. M., & Taylor, J. R. (2016). Neuroscience of learning and memory for addiction medicine: From habit formation to memory reconsolidation. Progress in Brain Research, 223. https://doi.org/10.1016/bs.pbr.2015.07.006
The first version of this page was posted January 18, 2005.